Select your destination
Continue to Radiometer Medical
Blood gas monitoring in the preterm neonate
Using transcutaneous monitoring (TCM) can help you protect and guide the treatment of the most fragile patients in the NICU [1,2]. TCM devices can be used in all stages of neonatal care — immediately after transition at birth, in the NICU, and during inter-hospital transfers [1,2].
Monitoring neonatal ventilation
Managing neonatal ventilation is a delicate balance: both too little and too much oxygen and carbon dioxide is harmful for the neonate, highlighting the importance of close ventilation monitoring and management.
Too high or low O2 and CO2 levels have been shown to be a risk factor for mortality, necrotizing enterocolitis (NEC), retinopathy of prematurity (ROP), bronchopulmonal dysplasia (BPD), intraventricular hemorrhage (IVH), and cerebral injury among others (Table 1).
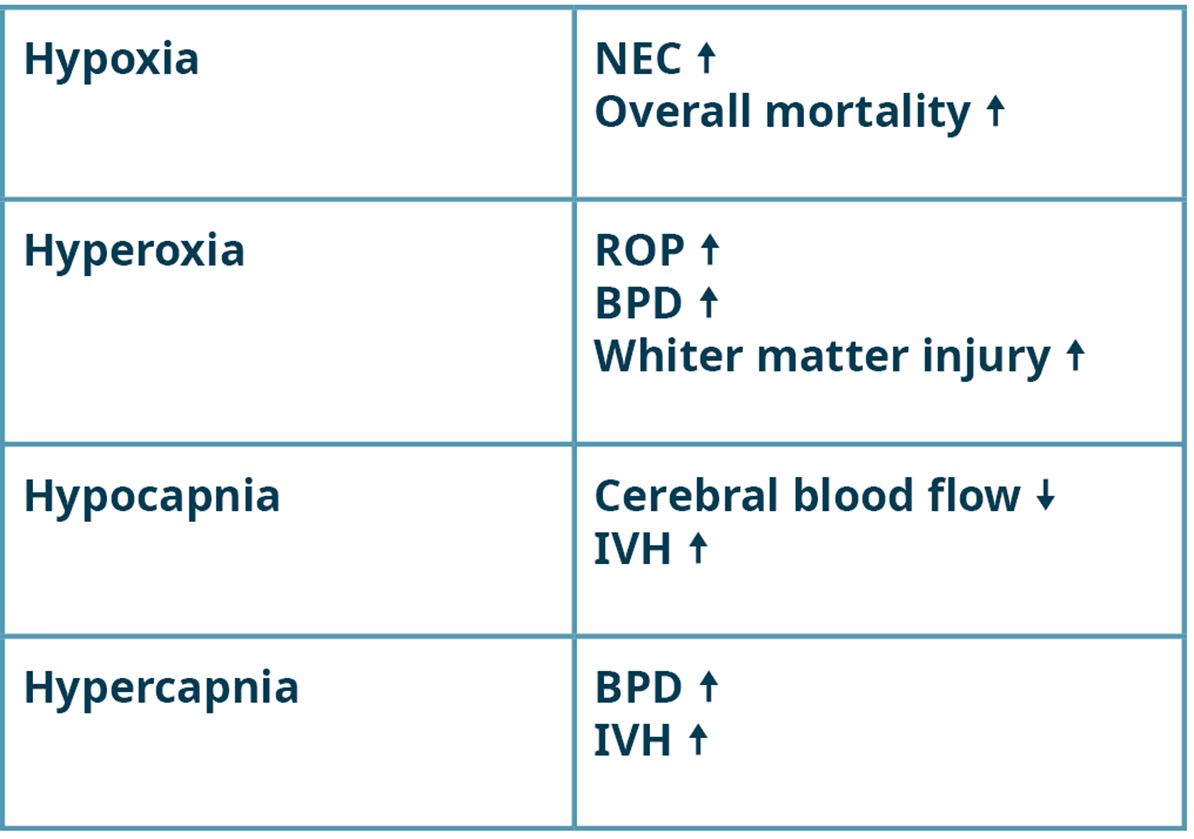
Table 1. Adverse effects of high and low O2 and CO2 levels in the neonate [3-7]
Managing neonatal ventilation can be achieved using invasive (blood gas) and non-invasive measurements (transcutaneous measurement, oxygen saturation measurement, end tidal measurement). Each method has its advantages and disadvantages and should optimally be used to supplement each other (Table 2)[3].
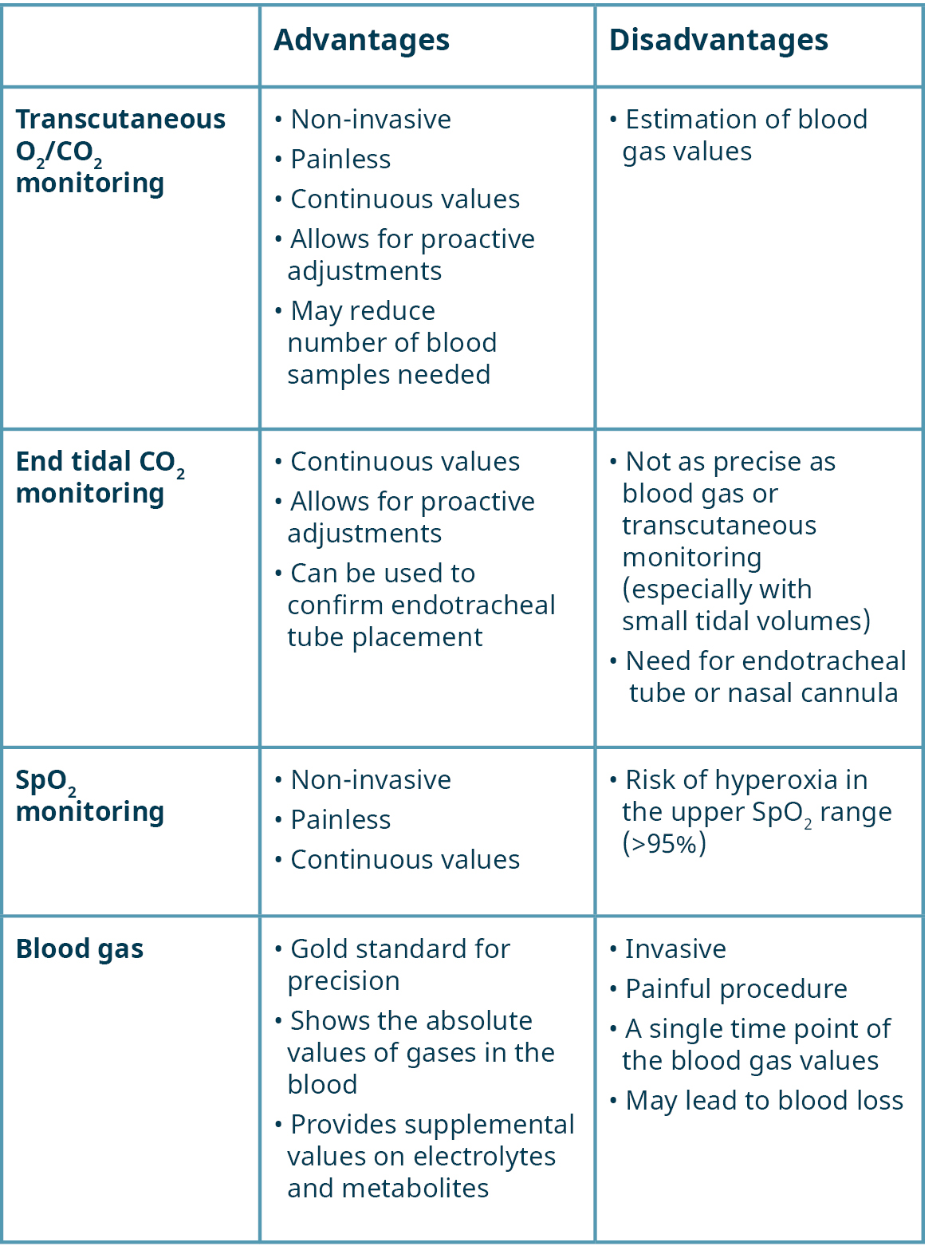
Table 2 – Advantages and disadvantages of different monitoring methods [8-11]
Blood gas analyses give the most precise measurement of O2 and CO2 values; however, they are invasive, can cause pain for the infant, induce blood loss, and may cause temporary disturbances in the cerebral blood flow [12]. Furthermore, the blood gas measurement only shows a single time point of the neonatal oxygenation and ventilation status and does not reflect the intermittent changes between two samples.
Oxygen saturation (SpO2) monitoring is used as standard of care for monitoring of oxygenation of neonates. It is non-invasive, instantaneous, and shows continuous values. Though SpO2 is good at detecting hypoxia, titration of ventilation can be difficult, with a risk of overlooking hyperoxia for SpO2 values ≥95-98% [8].
End-tidal CO2 (ETCO2) monitoring can be used to confirm endotracheal tube placement in neonates and can give continuous values for infants on a ventilator or with respiratory support [2]. It is generally not as precise as tcpCO2, especially for infants with respiratory disease and/or ventilation/perfusion mismatch, a situation commonly occurring in the NICU [2,10].
Transcutaneous measurement of oxygen (tcpO2) and carbon dioxide (tcpCO2) can be used as a supplement to blood gases to monitor oxygenation and ventilation status of neonates.
Using continuous tcpCO2 values allows for proactive rather that reactive treatment, and might be used to diagnose adverse events like pneumothorax earlier [13]. The transcutaneous values of CO2 has shown a good correlation with arterial values and can be used even for extremely premature (gestational age < 28 weeks) and extremely low birth weight (birth weight < 1000 grams) infants [14].
One study showed that tcpO2 was superior to SpO2 to guide titration of oxygen delivery to preterm neonates, with less time spent at high or low arterial oxygen tensions [15].
Reducing pain and blood loss
Research shows that the preterm infant may be subject to painful procedures several hundred times during the first weeks of life, with blood samples being the most common source of pain [16].
Using a non-invasive method to continuously evaluate the O2 and CO2 levels may reduce the number of painful procedures the preterm infant experiences. One center showed a 25% reduction in number of blood draws for ventilated preterm infants after introduction of transcutaneous CO2 monitoring [17].
Summary
Transcutaneous monitoring of O2 and CO2 is painless and non-invasive, feasible for even the smallest and most premature neonates, has shown good correlation with arterial values, and can help guide the clinician in optimizing ventilation settings within a large range of clinical settings.
References
1. Bresesti I, Bruckner M, Mattersberger C, Baik-Schneditz N,
Schwaberger B, Mileder L et al. Feasibilty of Transcutaneous pCO2 Monitoring During Immediate Transition After Birth-A Prospective Observational Study. Front Pediatr 2020; 8:11.
2. Hochwald O, Borenstein-Levin L, Dinur G, Jubran H, Ben-David S, Kugelman A. Continuous Noninvasive Carbon Dioxide Monitoring in Neonates: From Theory to Standard of Care. Pediatrics 2019; 144(1).
3. Sandberg KL, Brynjarsson H, Hjalmarson O. Transcutaneous blood gas monitoring during neonatal intensive care. Acta Paediatr 2011; 100(5):676–9.
4. Tarnow-Mordi W, Stenson B, Kirby A, Juszczak E, Donoghoe M, Deshpande S et al. Outcomes of Two Trials of Oxygen-Saturation Targets in Preterm Infants. N Engl J Med 2016; 374(8):749–60.
5. Subramanian S, El-Mohandes A, Dhanireddy R, Koch MA. Association
of bronchopulmonary dysplasia and hypercarbia in ventilated infants with birth weights of 500-1,499 g. Matern Child Health J 2011; 15 Suppl 1:S17-26.
6. Perrone S, Bracciali C, Di Virgilio N, Buonocore G. Oxygen Use in Neonatal Care: A Two-edged Sword. Front Pediatr 2017; 4(143).
7. Fabres J, Carlo WA, Phillips V, Howard G, Ambalavanan N. Both extremes of arterial carbon dioxide pressure and the magnitude of fluctuations in arterial carbon dioxide pressure are associated with
severe intraventricular hemorrhage in preterm infants. Pediatrics 2007; 119(2):299–305.
8. Bachman TE, Newth CJL, Iyer NP, Ross PA, Khemani RG. Hypoxemic and
hyperoxemic likelihood in pulse oximetry ranges: NICU observational study. Arch Dis Child Fetal Neonatal Ed 2019; 104(3):F274-F279.
9. Restrepo RD, Hirst KR, Wittnebel L, Wettstein R. AARC clinical practice guideline: Transcutaneous monitoring of carbon dioxide and oxygen: 2012. Respir Care 2012; 57(11):1955–62.
10. Duyu M, Mocan Çağlar Y, Karakaya Z, Usta Aslan M, Yılmaz S, Ören Leblebici AN et al. Comparison of arterial CO2 estimation by end-tidal and transcutaneous CO2measurements in intubated children and variability with subject related factors. J Clin Monit Comput 2020.
11. Huttmann SE, Windisch W, Storre JH. Techniques for the measurement and monitoring of carbon dioxide in the blood. Ann Am Thorac Soc 2014; 11(4):645–52.
12. Roll C, Hüning B, Käunicke M, Krug J, Horsch S. Umbilical artery catheter blood sampling decreases cerebral blood volume and oxygenation in very low birthweight infants. Acta Paediatr 2000;
89:862–6.
13. McIntosh N, Becher J-C, Cunningham S, Stenson B, Laing IA, Lyon AJ et al. Clinical diagnosis of pneumothorax is late: use of trend data and decision support might allow preclinical detection. Pediatr Res 2000; 48(3):408–15.
14. Sørensen LC, Brage-Andersen L, Greisen G. Effects of the
transcutaneous electrode temperature on the accuracy of transcutaneous carbon dioxide tension. Scand J Clin Lab Invest 2011; 71(7):548–52.
15. Quine D, Stenson BJ. Does the monitoring method influence stability of oxygenation in preterm infants? A randomised crossover study of saturation versus transcutaneous monitoring. Arch Dis Child Fetal Neonatal Ed 2008; 93(5):F347-50.
16. Cignacco E, Hamers J, van Lingen RA, Stoffel L, Büchi S, Müller R et
al. Neonatal procedural pain exposure and pain management in ventilated preterm infants during the first 14 days of life. Swiss Med Wkly 2009; 139(15-16):226–32.
17. Mukhopadhyay S, Maurer R, Puopolo KM. Neonatal Transcutaneous Carbon Dioxide Monitoring--Effect on Clinical Management and Outcomes. Respir Care 2016; 61(1):90–7.
Cookies are used on this website
Use of cookiesPlease enter a valid email
We will be sending an e-mail invitation to you shortly to sign in using Microsoft Azure AD.
It seems that your e-mail is not registered with us
Please click "Get started" in the e-mail to complete the registration process
Radiometer is using Microsoft AZURE Active Directory to authenticate users
Radiometer uses Azure AD to provide our customers and partners secure access to documents, resources, and other services on our customer portal.
If your organization is already using Azure AD you can use the same credentials to access Radiometer's customer portal.
Key benefits
- Allow the use of existing Active Directory credentials
- Single-sign on experience
- Use same credentials to access future services
Request access
You will receive an invitation to access our services via e-mail when your request has been approved.
When you accept the invitation, and your organization is already using AZURE AD, you can use the same credentials to access Radiometer's customer portal. Otherwise, a one-time password will be sent via e-mail to sign in.
