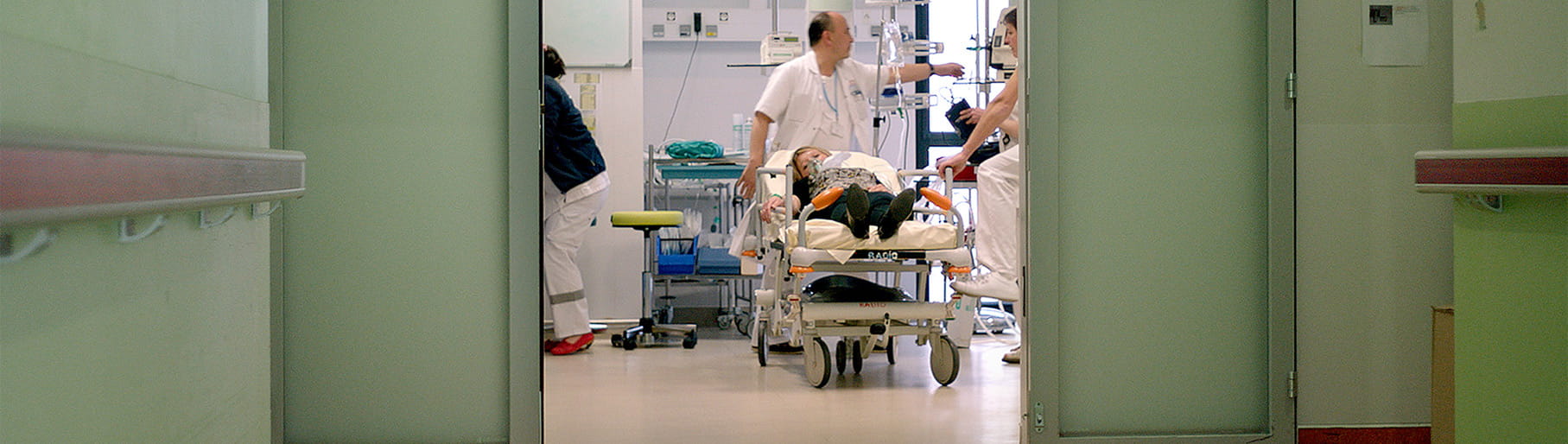
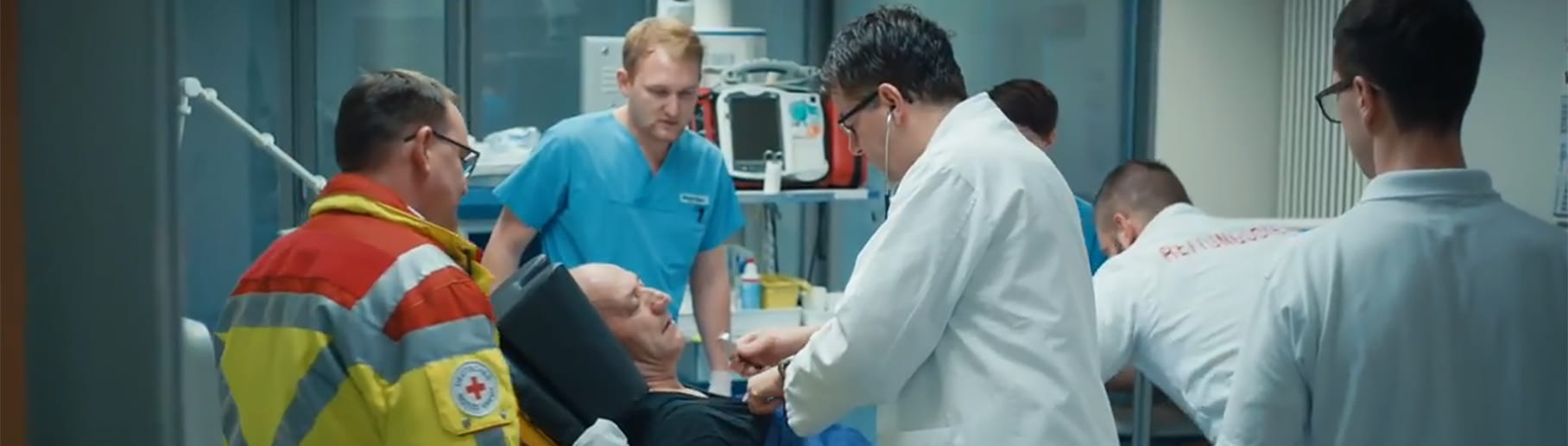
Select your destination
Continue to Radiometer MedicalRadiometer is using Microsoft AZURE Active Directory to authenticate users
Radiometer uses Azure AD to provide our customers and partners secure access to documents, resources, and other services on our customer portal.
If your organization is already using Azure AD you can use the same credentials to access Radiometer's customer portal.
Key benefits
- Allow the use of existing Active Directory credentials
- Single-sign on experience
- Use same credentials to access future services
Request access
You will receive an invitation to access our services via e-mail when your request has been approved.
When you accept the invitation, and your organization is already using AZURE AD, you can use the same credentials to access Radiometer's customer portal. Otherwise, a one-time password will be sent via e-mail to sign in.
Effective Date January 20th, 2023 (last updated January 20th, 2023)
ABOUT THIS POLICY
Radiometer values your privacy and the protection of your personal data. This policy (“Policy”) explains how Radiometer its affiliates, subsidiaries or related companies, a full list of which can be located here (together, “Radiometer”, “our”, “us”, or “we”), collects, uses, shares, transfers and processes data collected from or about you.
“Personal Data” is any information that can be used to directly or indirectly identify an individual or that can be reasonably expected to link to an individual. This can include items such as name, address, telephone number, credit card details, email address, ID number, Internet Protocol (“IP”) address of an electronic device used by an individual, or other identifying code (even absent of other identifying information). Statistical and non-identifiable metric data are not considered Personal Data.
The Radiometer subsidiary, affiliate or related company with which you interact is, where applicable, the data controller (or equivalent under applicable law) responsible for the processing of your Personal Data. You can find a list of the relevant legal entities that act as data controllers in Appendix 1 to this Policy.
SCOPE
This Policy describes the types of Personal Data that we may collect, process or disclose about you and how you may govern this processing by exercising applicable legal rights. This Policy applies to both online and offline information collection, including your use of websites or subdomains operated by us, any mobile applications, when we provide products and/or services to you or notify you about prospective items of interest and in other situations where you interact with us in-person, by telephone or by mail where this Policy is posted or referenced.
There may be occasion where you have been provided with a circumstance-specific privacy notice that is separate from this policy, such as privacy notices for specific activities such as Recruitment. To the extent you were provided with a different notice, those notices apply and govern our interactions with you. If you provide Personal Data about parties other than yourself, you are responsible for ensuring their knowledge of how we will process their personal data, and, where applicable, obtaining any necessary consents required in advance.
We are committed to processing Personal Data in accordance with applicable laws. Please note that if you do not wish to provide your Personal Data to us, some products and/or services may become unavailable to you. Your use of any or all these platforms indicates you have been notified of our collection, use, transfer, and disclosure of your information as described in this Policy to the extent permitted by applicable law.
Read more